Tags
Dartmouth Atlas, Health care, Hip Replacement, joint replacement, knee replacement, Lincoln Journal Star, Sports Medicine, surgery
Lincoln knee replacement rates bend to patient demand
By MARK ANDERSEN / Lincoln Journal Star | Posted: Monday, July 18, 2011 9:00 am
A decade ago, it was nearly unknown for someone in their 40s or 50s to get a replacement knee or hip.
For a variety of reasons — patient demand being a big reason — it’s become commonplace.
In 2005, 23 percent of patients undergoing knee or hip joint replacement surgery at Saint Elizabeth Regional Medical Center were younger than 65. Last year, 37 percent were younger.
About 1,000 joint replacements are done at Saint Elizabeth every year, 40 percent of hip and knee patients men, compared to 32 percent in 2005.
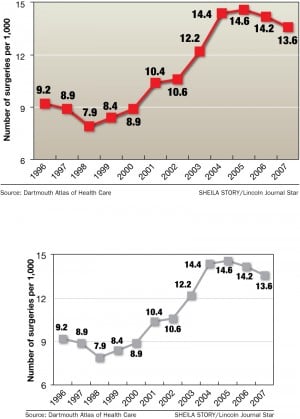
Younger and male patients have added to a local joint replacement boom already occurring among the retired set. Between 1997 and 2007, hip replacements among Medicare patients in the Lincoln hospital referral market climbed from 3 to 4 per 1,000 patients, according to the Dartmouth Atlas of Health Care. Knees climbed from 9 per 1,000 to 14.
Knees are the bigger story.
Hip replacements were the more common procedure until about a decade ago, said Dr. James Gallentine of Nebraska Orthopedic and Sports Medicine, but knees shot past and now lead by a furlong.
A Journal of Arthroplasty article predicts there will be national demand for 418,000 hip replacements in 2016, while demand for knees will climb above 1.2 million. By 2030, trends suggest, annual demand for replacement knees will climb to 3.8 million, with the implants alone costing an estimated $50 billion.
In terms of pain relief, hip replacements require less justification. Hip arthritis is truly debilitating.
“They’re miserable,” Gallentine said. They can’t do anything.
Among the elderly, he said, hip replacement is far cheaper than nursing home care.
Bad knees hurt, and sometimes a lot, he said, but it’s not as debilitating.
* * *
Bob Keller, 61, had his left hip replaced in October after enduring 18 months of pain so bad it kept him up nights. The Lincoln manufacturing manager spends 80 percent of his day on his feet, and a foreign growth on his hip socket felt like “an abscessed tooth in your hip.”
He spent two months considering surgery that ultimately, “for me, was a snap. I was in the hospital for three days and on my feet the day after. … Pain-wise, I have none.”
* * *
The trend toward younger, male and overall more knees brings relief to many joint pain sufferers, but it carries worrisome implications.
By 2016, predicts the Journal of Arthroplasty study, a national shortage of bone surgeons will cause 230,000 knee replacement surgeries to go undone every year — that’s the conservative estimate.
With younger patients getting knee surgery, Nebraska Orthopedic’s Gallentine also foresees increased demand for revisions — surgical replacement of artificial joints due to worn plastic parts, shortened bones or infections.
Revisions can cost considerably more, and they come with more complications, more stiffness and higher infection rates.
“Everything bad is up,” Gallentine said.
Worry over revisions is why physicians commonly have advised patients to delay knee replacement. The younger the patient, the greater the odds they’ll outlive their first artificial joint.
It’s estimated 95 percent of artificial joints will be functional in 15 years, Gallentine said, but it may be only 85 percent. The nation’s artificial joint registry isn’t reliable, he said. Meanwhile, people live into their 80s.
Plastic parts have improved, he says, but shearing forces exerted on artificial knees surely will test them.
Many things have contributed to the growing demand for knees, Gallentine said, but nothing medical fully explains it.
There are more aging boomers and more people overweight, which exacerbates joint wear. Together, he said, weight and age explain about half the increase in demand.
The remainder appears patient driven, he said. There’s been a cultural shift.
***
In January, LaVerle Miller, 50, had surgery to replace a knee seriously injured while playing softball years earlier.
The York agricultural company salesman had felt it getting worse over time. He eventually quit running.
For the last three or four years, he said, “every time I took a step, it burned.”
His research into the various types of replacement knees brought him to Nebraska Orthopedic, where he heard the message: You’re young, but you’ll know when the pain is bad enough. You’ll know when you want it done.
That moment came in San Diego during a Cornhuskers game when he struggled to keep up. Miller increased his flex spending contributions and set surgery for early this year.
The pain and rehabilitation was, “probably not as bad as I thought it would be,” he said. He’s playing golf again.
The new knee could last 20 or 30 years, but he also knows he might need a replacement.
But there was no way he was waiting. It hurt that bad.
“Maybe 10 years down the road,” he adds, “they’ll have something else.”
Miller is happy with his decision, and, he adds, so is his wife.
***
Lincoln may be a national bellwether when it comes to the nation’s changing knee surgery attitudes.
The Lincoln hospital market led the nation from 2003 to 2006 in rates of knee replacement surgeries among Medicare patients. It fell to second place in 2007, the last year listed by the Dartmouth Atlas.
Surgical techniques have improved, Gallentine said. Hospital stays have fallen from two weeks to a few days.
And the implants do work for most people, he said.
More and more, the people who come in with knee pain already know they want a new knee.
It’s increasingly likely they already know someone who underwent surgery at a younger age.
The conclusion of the Journal of Arthroplasty study: “We predict a supply-side crisis that severely threatens access for our arthritic patients.”
Reach Mark Andersen at 402-473-7238 or [email protected].
Read more: http://journalstar.com/news/local/article_b71c4ce2-74a3-55d0-b9cc-149ae14b1a58.html#ixzz1SuQ5dcvR
Related articles
- Pain in knee after total knee replacement a year ago. What are the options? (zocdoc.com)
- Men Who Smoke at Lower Risk of Joint Replacement (nlm.nih.gov)

Pingback: As Baby Boomers Age, Orthopedic Surgeons Will See More Demand « Earl's View
Pingback: Obese Are Three Times as Likely to Need a Hip or Knee Replacement « Earl's View
Pingback: Sydney Orthopaedic Specialists give the “good oil” on Knees « Earl's View
Pingback: Baby boomer injuries booming « Earl's View
Pingback: As baby boomers age, joint replacements soar « Earl's View
Pingback: First Blended Vitamin E Total Knee Replacement in the United States « Earl's View
Pingback: What To Consider Before Joint Replacement Surgery « Earl's View
Pingback: Joint Replacement Surgery Increases Risk of Blood Clot Formation in Certain Patients « Earl's View
Pingback: Advances in Knee Replacement Surgery for Active Baby Boomers « Earl's View
Pingback: Hip & Knee Replacement Numbers Skyrocketing – Baby Boomers Get Old « Earl's View
Pingback: Tiger Woods: Why a knee replacement is out… « Earl's View
Pingback: Chuck Molnar, Senior Corner: Knee replacement worth the anxiety « Earl's View
Pingback: Knee Replacement Surgery « Earl's View
Pingback: Facts About Joint Replacements « Earl's View
Pingback: Zimmer Knee Replacement Lawsuit « Earl's View
Pingback: Hospital “looses” Urgent Hip Replacement Paperwork for Former Nurse « Earl's View
Pingback: Zimmer Knee Replacement for Women « Earl's View
Pingback: What Is A Knee Replacement Surgery? « Earl's View
Pingback: Joint effort: Replacements becoming more popular « Earl's View
Pingback: New Zealand National Joint Registry Eleven Years Data Jan 1999 – 2009 « Earl's View
Great information shared..! Liked your blog.
Thanks!