Tags
Food & Drug Administration, Glenohumeral joint, Hip Replacement, joint replacement, Reverse Total Shoulder Replacement, Rotator cuff, Shoulder replacement, surgery, UNited States
Since it was first approved by the FDA for broad use in the United States in 2004, reverse shoulder arthroplasty has given new hope to patients suffering from severe arthritis or other degrading shoulder disorders.
 Photo: “Rotator cuff repair is difficult; the blood supply to the rotator cuff is poor, so it doesn’t always heal well,” Dr. Sabesan says. Photo courtesy of MSU/KCMS, by Will Panich Photography
Photo: “Rotator cuff repair is difficult; the blood supply to the rotator cuff is poor, so it doesn’t always heal well,” Dr. Sabesan says. Photo courtesy of MSU/KCMS, by Will Panich Photography
Yet the rotator cuff, a key component to successful outcomes, continued to present challenges for the orthopedic surgeon.
Today, thanks to experience gained from seven years of surgical outcomes — from new research and advances in the body of knowledge surrounding this complex joint and muscle group — surgeons like Vani Sabesan, M.D., Michigan State University Kalamazoo Center for Medical Studies (MSU/KCMS), can achieve unprecedented functionality for patients.
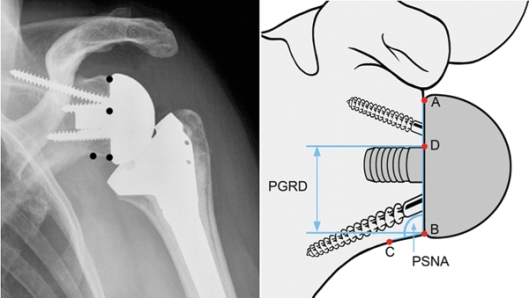 “Even though shoulder pain and a loss of shoulder function are problems that affect a significant number of patients, until recently, our treatment options were limited and our progress lagged behind advances in hip and knee surgeries because the shoulder joint is so much more complex,” says Dr. Sabesan, an expert in complex shoulder disease.
“Even though shoulder pain and a loss of shoulder function are problems that affect a significant number of patients, until recently, our treatment options were limited and our progress lagged behind advances in hip and knee surgeries because the shoulder joint is so much more complex,” says Dr. Sabesan, an expert in complex shoulder disease.
As Americans age, musculoskeletal disorders are an increasing problem. Joint replacements in all categories continue to increase. The number of shoulder replacements, however, has consistently lagged behind hip and knee replacements.
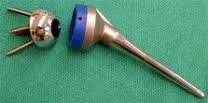 “Today, total shoulder replacements have been shown to be comparable to both hip and knee surgeries in terms of success, pain relief and functional improvement, but this isn’t commonly recognized because not as many procedures have been performed,” says Dr. Sabesan. “Most people know someone — a relative or a friend — who has had a hip or knee replaced. The same can’t be said for shoulder replacements, but that is quickly changing as these procedures become more common. Today, shoulder replacement surgery is a viable and increasingly popular choice for patients with shoulder pain.”
“Today, total shoulder replacements have been shown to be comparable to both hip and knee surgeries in terms of success, pain relief and functional improvement, but this isn’t commonly recognized because not as many procedures have been performed,” says Dr. Sabesan. “Most people know someone — a relative or a friend — who has had a hip or knee replaced. The same can’t be said for shoulder replacements, but that is quickly changing as these procedures become more common. Today, shoulder replacement surgery is a viable and increasingly popular choice for patients with shoulder pain.”
Despite the increasing number of patients helped through shoulder arthroplasty, some remained beyond help due to a damaged rotator cuff. According to the National Ambulatory Medical Care Survey 1998-2006, the most recent data available, nearly 7.5 million physician visits in 2006 were due to shoulder problems. Of those, more than 4.1 million were for rotator cuff problems, specifically, and the problem is slated to increase because it is associated with aging.
“Through research, by examining cadavers of people in their 80s and older, we’ve found that more than 50% had at least some rotator cuff pathology,” Dr. Sabesan says.
 In a healthy shoulder, an intact rotator cuff and its surrounding muscles keep the joint centered and help lift the shoulder, allowing it to move. Rotator cuff disorders range from mild arthritis to rotator cuff tear arthropathy, a severe and complex form of shoulder arthritis. When this occurs, the cartilage that normally covers the joint surface is no longer intact. As a result, the tendons that help position and move the joint are unable to function properly, even with a prosthetic joint.
In a healthy shoulder, an intact rotator cuff and its surrounding muscles keep the joint centered and help lift the shoulder, allowing it to move. Rotator cuff disorders range from mild arthritis to rotator cuff tear arthropathy, a severe and complex form of shoulder arthritis. When this occurs, the cartilage that normally covers the joint surface is no longer intact. As a result, the tendons that help position and move the joint are unable to function properly, even with a prosthetic joint.
“Rotator cuff repair is difficult; the blood supply to the rotator cuff is poor, so it doesn’t always heal well,” Dr. Sabesan says.
The reverse shoulder arthroplasty is a solution that directly addresses chronic deficiencies of a torn rotator cuff, compensating for its weakness or absence by rearranging the anatomy.
“In this procedure, the ball portion of the joint is taken from the humerus side and moved to the shoulder blade or scapula side and attached with an implant or prosthesis. The socket is moved to the upper end of the humerus side,” says Dr. Sabesan. “No other joint replacement surgery changes the normal anatomical structure like this.”
Like traditional shoulder replacement surgeries, the arthritic joint surfaces are replaced with a highly polished metal ball attached to a plastic socket, but in the reverse procedure, the socket and metal ball are switched. The reverse procedure constrains the ball in a cup that is inserted into the end of the humerus, and the metal ball is attached to the shoulder bone. The reversal increases tension of the deltoid muscle, producing more torque. In this way, the deltoid muscle compensates for the loss of rotator cuff by becoming the primary elevator of the shoulder joint and making it easier for a patient to raise his or her arm. Yet, range of motion remains limited.
“The instrumentation and tissue allograph options continue to improve, along with our understanding of the biology of the shoulder,” says Dr. Sabesan. “We can now use these allographs to augment the remaining muscle. We’re now using more platelet-rich plasma — plasma that contains higher than physiologic platelet content than normal plasma — to accelerate tissue and wound healing. These advancements enable us to provide treatment options that weren’t available to patients as recently as a few years ago,” says Dr. Sabesan.
Dr. Sabesan cautions, however, that although the technology is exceptional, it is not for every patient. Appropriate patient selection is essential to achieving the best outcomes.
Indications for the reverse total shoulder arthroplasty include patients with debilitating arthritis and irreparable rotator cuff damage, as well as for a revision of a previously failed conventional total shoulder arthroplasty in which the rotator cuff tendons are degraded or otherwise damaged.
“Today, indications for reverse shoulder arthroplasty are an older patient with a lower activity lifestyle,” Dr. Sabesan says. “Based on our knowledge and understanding of the outcomes, the ideal population tends to be patients between the ages of 60 and 70 years old. In some cases, the age may be younger, but that would be true only for someone with a lower-impact lifestyle because the lifting capacity of the shoulder will be decreased with a reverse arthroplasty.”
Within this population, the procedure is also being used for the treatment of fractures or breaks in the proximal humerus bone.
“That’s been a significant area of growth for the reverse shoulder arthroplasty and is a condition that we really hadn’t considered for this procedure in the past,” Dr. Sabesan says. “Before, we would have tried to plate or replace the bone, but the outcomes were still very poor in terms of function and healing of the muscles. The reverse arthroplasty generally improves outcomes for these patients now.”
Dr. Sabesan says conditions common to aging that affect the shoulder, such as osteoporosis and arthritis, don’t have to be lifestyle inhibitors anymore, and that makes her work more rewarding.
“We have a large population of older citizens who lead active lives in our region,” says Dr. Sabesan. “The advances that we are seeing in shoulder repair, joint replacement and even reverse shoulder arthroplasty can keep them active. It can also help others who may be faced with lifestyle limitations achieve renewed function without pain, but we need to tell them these options are available.”
Dr. Sabesan is at the forefront of research within this field. She is leading efforts to study the shoulder joint using 3-D modeling software and imaging scans to better understand shoulder disease and dysfunction to improve patient outcomes.
“The shoulder joint has so many planes of movement that it has been much harder to develop effective replacement prostheses, especially if a patient’s condition is further complicated by torn muscles,” Dr. Sabesan explains. “It is this very complexity that makes continued research so essential. It is also why recent advancements in this field are so exciting. When you consider the potential number of patients who may benefit from these advancements, this branch of orthopedic surgery has the potential to change the way our society ages.”
Dr. Sabesan cites a patient with a broken proximal humerus by way of example.
“This patient had received a hemi arthroplasty, a partial shoulder replacement, four years ago,” Dr. Sabesan explains. “This patient, however, did not regain much function. Her shoulder was weak, and she had frequent pain. Yet, she did not realize that there were new procedures available to her that would directly address these lifestyle challenges. Today, she has regained much more strength and functionality and is relatively pain-free as a result of a reverse shoulder arthroplasty I performed.”
A few years from now, this patient and others like her are apt to discover that treatment options have continued to progress thanks to Dr. Sabesan’s ongoing commitment to improving treatments for complex shoulder disorders.
“It is very exciting to be in a position to help advance this research,” says Dr. Sabesan. “It wouldn’t be possible without the resources and leadership that exist in our community, at MSU/KCMS and specifically within the orthopedic program here.
I believe it is institutions like MSU/KCMS that will have the greatest impact on the future of health care. Here, not only do we have the opportunity to work at two great hospitals, but we also have the support of an organization that is committed to addressing these important issues through practice, research and the education of the next generation of doctors.”
About Dr. Sabesan
 Vani Sabesan, M.D., received her medical degree from Indiana University School of Medicine. Concurrently, she completed a Doris Duke Clinical Research Fellowship in orthopedic surgery at The University of Iowa. Following medical school, she completed her residency in orthopedic surgery at Duke University Medical Center in Durham, NC, followed by a shoulder and elbow surgery fellowship at the Cleveland Clinic. She joined Michigan State University Kalamazoo Center for Medical Studies in October 2010. Dr. Sabesan specializes in complex shoulder and elbow disease and sports medicine and is implementing a specialty clinic to identify, evaluate, educate and treat patients who suffer from osteoporosis and have or are at risk for fragility fractures.
Vani Sabesan, M.D., received her medical degree from Indiana University School of Medicine. Concurrently, she completed a Doris Duke Clinical Research Fellowship in orthopedic surgery at The University of Iowa. Following medical school, she completed her residency in orthopedic surgery at Duke University Medical Center in Durham, NC, followed by a shoulder and elbow surgery fellowship at the Cleveland Clinic. She joined Michigan State University Kalamazoo Center for Medical Studies in October 2010. Dr. Sabesan specializes in complex shoulder and elbow disease and sports medicine and is implementing a specialty clinic to identify, evaluate, educate and treat patients who suffer from osteoporosis and have or are at risk for fragility fractures.
Related articles
- Future of Hip replacement may include more resurfacing, percutaneous fixation (earlsview.com)
- Robert Zanotti, MD, Is First Lorain County, Ohio Orthopedic Surgeon to Perform Reverse Total Shoulder Replacement (prweb.com)
- Baby Boomers And Joint Replacement Surgery – Pathology perspectives (hofholistichealingcenters.wordpress.com)
- UK – Advice for GP’s – Hip Joint Replacements (earlsview.com)
- Bio-Engineering – Need a new hip? Someday you may grow your own… (earlsview.com)
- Tornier Announces First Implant in U.S. Trial of Its Simpliciti Stemless Shoulder Joint Replacement System (medgadget.com)
- Shoulder pain: Why you must see an Asheboro orthopedic doctor (bestmedicalpractices.wordpress.com)
- 7 Critical Orthopedic and Spine Device Industry Trends (earlsview.com)
- Joint Replacement Surgery – Patient Story … (earlsview.com)
- Operative time, use of biological agents increase risk of complications following TKA (earlsview.com)
- Hip resurfacing surgery India- Venkatachalam, British patient story (earlsview.com)
- Birmingham Hip Resurfacing or Surface Replacement Arthroplasty (BHR) With Stem (earlsview.com)
- Techniques In Implementing A Hip Replacement Operation (earlsview.com)
- New Zealand National Joint Registry Eleven Years Data Jan 1999 – 2009 (earlsview.com)

Pingback: Frozen shoulder « Community Care ::: Affordable Therapy Collect
Pingback: Orthopedists liable under federal anti-kickback statute « Earl's View
Pingback: Medical Tourism At Home: Big Companies Start to Shop at Hospitals Across the U.S. « Earl's View
Pingback: Shoulder Pain Treatment, Rotator Cuff Injury Treatment – Shoulder Pain NO MORE! | HealthAndFitnessCure.com
Pingback: Shoulder Pain Treatments Are the key to get rid of Pain and Anti Inflammatorie | The Back Pain Shoulder And Neck Pain Blog
Pingback: Physiotherapy For Your Shoulder | Shoulder Blade Pain Site